Brain Haemorrhage: A Complete, Actionable Guide
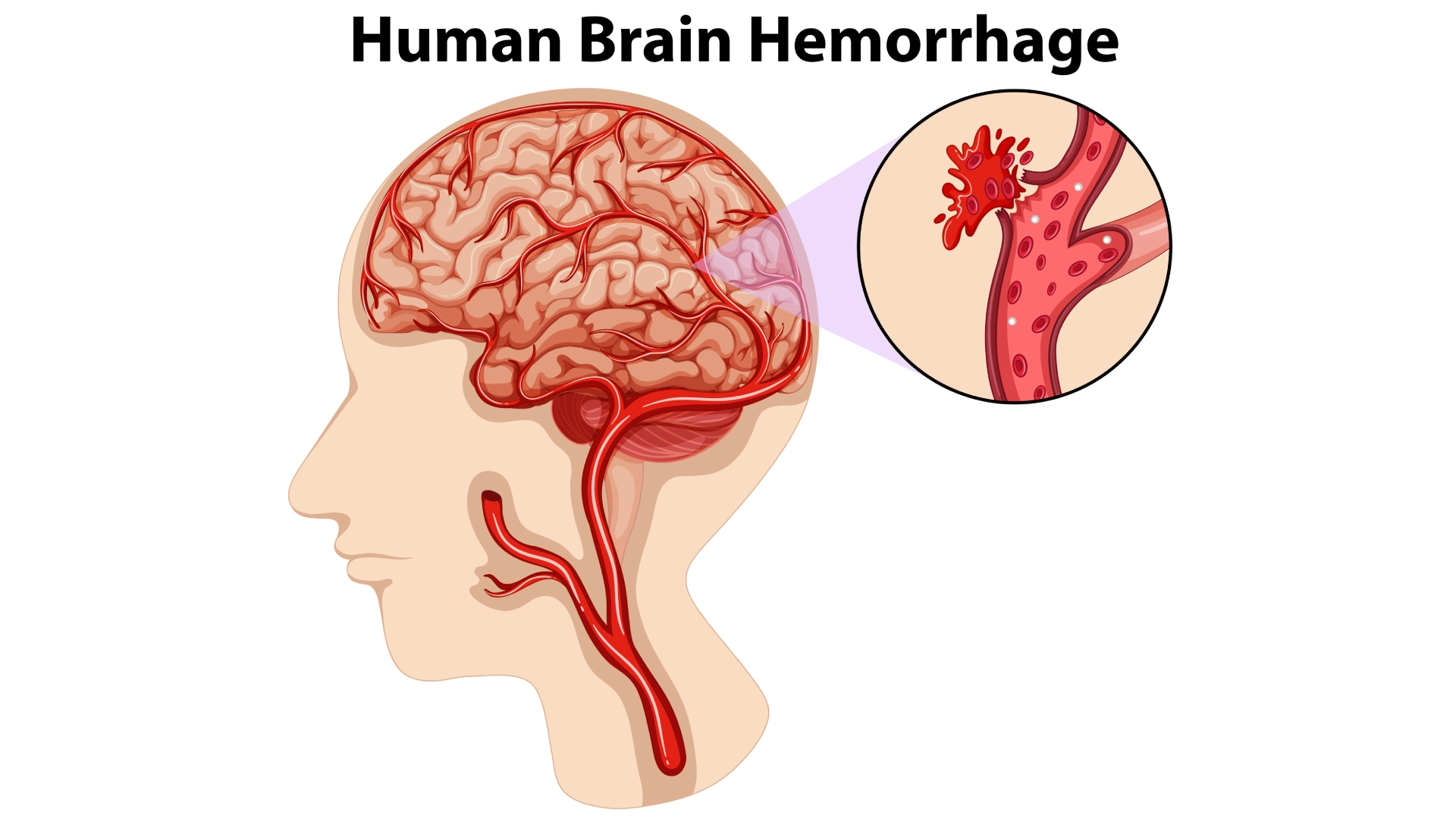
Sudden, severe headaches, confusion, weakness, or loss of consciousness—these may signal a brain haemorrhage, a medical emergency that requires immediate attention. Also known as intracranial haemorrhage, this condition refers to bleeding within the skull that compresses brain tissue and disrupts normal brain function.
Understanding what it is, why it happens, and how to respond can save lives. This guide breaks it down in clear, patient-friendly terms.
What Is a Brain Haemorrhage?
A brain haemorrhage occurs when a blood vessel inside the brain ruptures and bleeds. This bleeding increases pressure within the skull, compresses surrounding brain tissue, and interferes with oxygen and nutrient delivery to neurons.
Unlike a stroke caused by a blood clot (ischemic stroke), a haemorrhagic stroke involves bleeding into brain tissue, making it a distinct and often more serious form of stroke.
Types of Brain Haemorrhage
Understanding the type helps clinicians tailor treatment:
1. Intracerebral Haemorrhage
Bleeding occurs within the brain tissue itself. It is the most common form and often linked to high blood pressure.
2. Subarachnoid Haemorrhage
Bleeding occurs in the space between the brain and the thin tissues covering it (meninges). Often caused by a ruptured aneurysm.
3. Subdural and Epidural Haemorrhages
These occur between the skull and brain covering (dura), typically after head trauma.
Each type may have different symptoms, onset patterns, and urgency levels.
What Causes Brain Haemorrhage?
Several factors can weaken blood vessels or increase risk:
- High blood pressure (hypertension): Most common contributor.
- Head injury or trauma: Falls, collisions, and accidents.
- Aneurysms: Weak spots in vessel walls that can rupture.
- Arteriovenous malformations (AVMs): Tangled vessels prone to bleeding.
- Blood thinners (anticoagulants): Increase bleeding risk.
- Bleeding disorders: Such as hemophilia or liver disease.
Sometimes, the cause may be unknown until imaging is done.
Recognizing Symptoms: Know the Signs
Symptoms may appear suddenly or worsen rapidly and can vary by location and size of the bleed:
- Sudden, severe headache (“worst ever”)
- Weakness or numbness on one side of the body
- Difficulty speaking or understanding speech
- Loss of balance or coordination
- Vision changes
- Confusion, drowsiness, or loss of consciousness
- Seizures
If symptoms develop suddenly, especially with headache and weakness, treat it as an emergency.
Diagnosis: What to Expect at the Hospital
Brain haemorrhage requires rapid, definitive assessment:
- Neurological exam: Checks strength, reflexes, speech, eye movement.
- Brain imaging (CT scan or MRI): Quickly identifies bleeding location and extent.
- Angiography: May be used to find aneurysms or vessel abnormalities.
- Blood tests: Assess clotting factors and underlying risks.
Early imaging distinguishes haemorrhage from other types of stroke and guides treatment plans.
Treatment: Stopping the Bleed and Saving Brain Tissue
Treatment depends on the cause, size of the bleed, symptoms, and overall health:
Immediate care
- Stabilization: Ensuring breathing and blood pressure control.
- Medication: To reduce swelling, prevent seizures, or lower blood pressure.
Surgical intervention
- Craniotomy: Removing a portion of skull to relieve pressure and stop bleeding.
- Clipping/coiling of aneurysms: Prevents re-bleeding.
- Evacuation of hematoma: Removes pooled blood if necessary.
Rehabilitation
After initial treatment, therapies help patients recover lost skills:
- Physical therapy
- Speech and language therapy
- Occupational therapy
Recovery may take weeks to months and often depends on how quickly treatment began.
When Every Minute Matters
Brain haemorrhage is a medical emergency. The sooner bleeding is controlled and pressure relieved, the better the chance of minimizing brain damage and disability. If you see someone with sudden neurological symptoms, act immediately:
Call emergency services right away. Prompt response saves lives and preserves brain function.
Prevention: Lower Your Risk
While not all causes are preventable, many risk factors are modifiable:
- Control high blood pressure — the leading risk factor for intracerebral haemorrhage.
- Avoid tobacco and limit alcohol consumption.
- Manage chronic conditions such as diabetes and high cholesterol.
- Use protective gear in activities with fall or trauma risk.
- Discuss medication risks (especially blood thinners) with your clinician.
Regular health check-ups and risk assessment are powerful preventive tools.
Bottom Line: Awareness, Action, and Care
Brain haemorrhage can strike suddenly, but understanding its causes, symptoms, and treatments empowers you to act quickly. Early recognition and immediate medical care significantly improve outcomes. Whether through lifestyle changes, risk management, or emergency response, knowledge gives you an edge in protecting brain health.
